Treatments for varicose veins and venous insufficiency have become less invasive over the last decade. A number of different procedures are now possible most involving local anaesthetic or requiring no anaesthetic at all. Rather than remove all the faulty veins, which was done in traditional surgery, the newer techniques aim to block or "ablate" the faulty veins. This can have the same benefit in terms of vein function, but is less invasive.
FOAM SCLEROTHERAPY
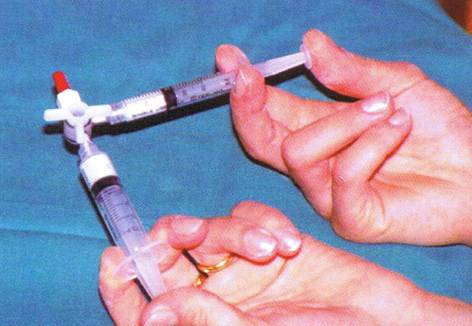 Some chemical agents when injected into veins cause them to become inflamed, and with time, scarring occurs leading to obliteration of the vein. Veins with faulty valves and varicisoites can be treated in this way. This is called sclerotherapy and has been practised for many years. Mixing the chemicals with air to make a foam is a more recent development which gives better results. Modern ultrasound can be used to direct the foam into the correct vein also improving results. Foam sclerotherapy can be performed in a clinic and does not require any anaesthesia. Following the treatment it is important to wear a bandage and/or a support stocking on the leg for 2 weeks. Success rates are approximately 70 – 80%. If the veins do not disappear the treatment can be repeated. Side effects can be due to reactions to the foam entering the general circulation. With care these reactions are uncommon and transient. Local “phlebitis” of the treated vein (inflamed thrombosis) can cause pain for 1-2 weeks and may occasionally leave some marking on the leg.(10-15%).
Some chemical agents when injected into veins cause them to become inflamed, and with time, scarring occurs leading to obliteration of the vein. Veins with faulty valves and varicisoites can be treated in this way. This is called sclerotherapy and has been practised for many years. Mixing the chemicals with air to make a foam is a more recent development which gives better results. Modern ultrasound can be used to direct the foam into the correct vein also improving results. Foam sclerotherapy can be performed in a clinic and does not require any anaesthesia. Following the treatment it is important to wear a bandage and/or a support stocking on the leg for 2 weeks. Success rates are approximately 70 – 80%. If the veins do not disappear the treatment can be repeated. Side effects can be due to reactions to the foam entering the general circulation. With care these reactions are uncommon and transient. Local “phlebitis” of the treated vein (inflamed thrombosis) can cause pain for 1-2 weeks and may occasionally leave some marking on the leg.(10-15%).
Mechanico-chemical vein ablation is where the sclerosant chemical is delivered directly into the faulty saphenous vein trunk with a catheter that also physically spins and slightly damages the lining of the vein. This combination is desgined to increase the success rate for obliterating the vein. The potential advantage of this is that it is less uncomfortable and needs less local anaesthetic than the thermal techniques (see next section). The long term durability is still being evaluated for this technique.
Endothermal Ablation
EndoVenous Laser Ablation (EVLA) and Readiofrequency Ablation (RFA) are techniques for treating varicose veins. These procedures seal off the main underlying faulty vein that is feeding the varicosities. This will be either the Long saphenous Vein (LSV) in the thigh or the Short Saphenous Vein (SSV) behind the knee and calf. The traditional operation was to tie and strip these veins. These ablation techniques have replaced that surgery and are less painful with quicker recovery.
EVLA and RFA are techniques to remove the LSV and SSV from the circulation without a wound and without stripping. Both these treatments can be performed under local anaesthesia. A catheter is passed up the vein from the ankle or knee level. It is carefully placed at the junction between the LSV/SSV and the deeper veins. An ultrasound scan is used to place the catheter precisely.
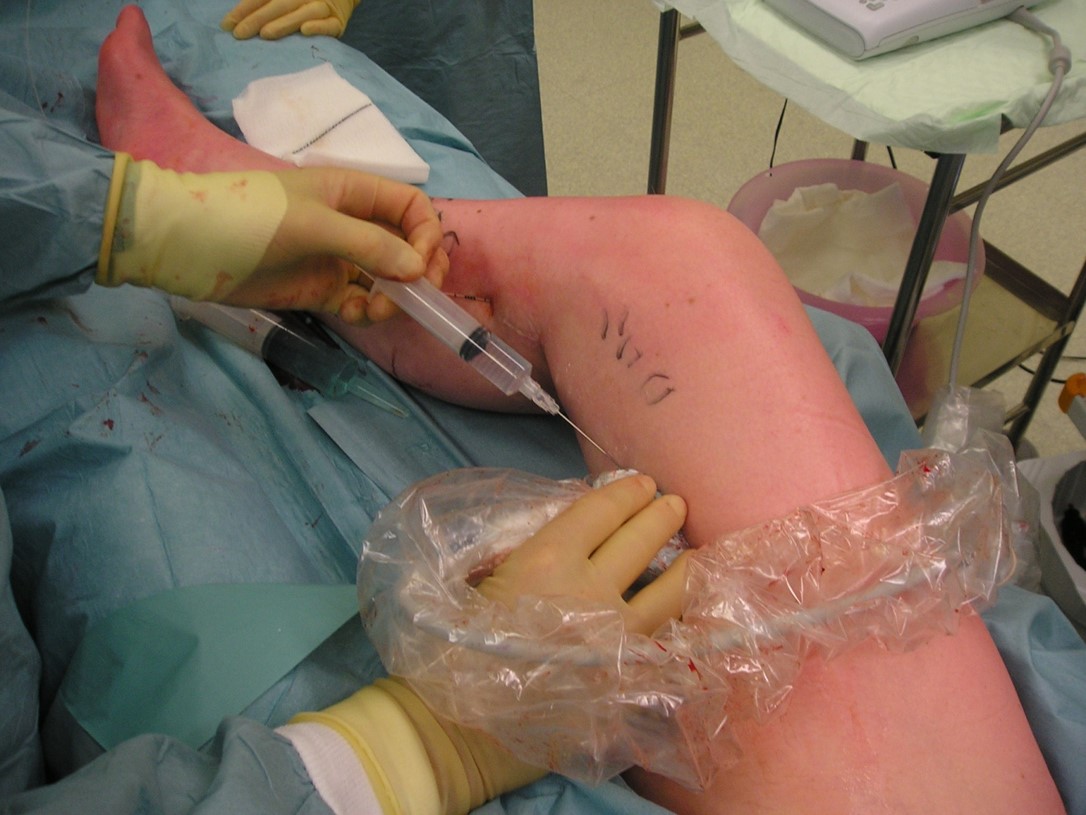
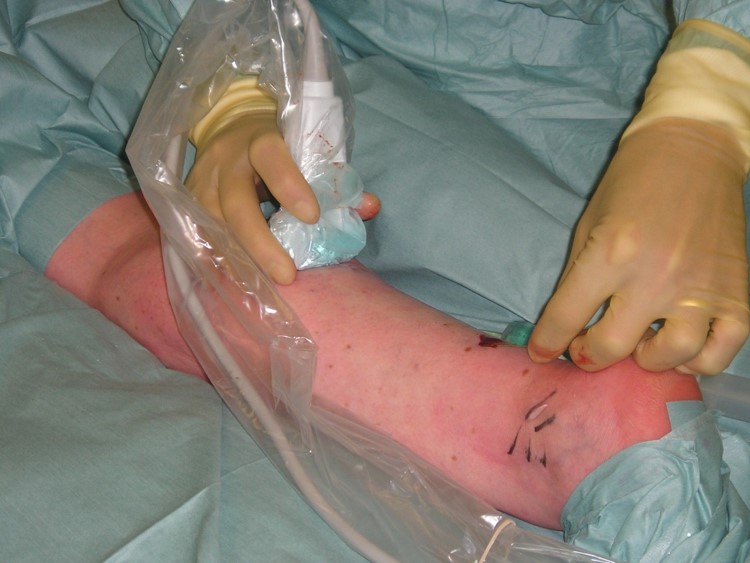
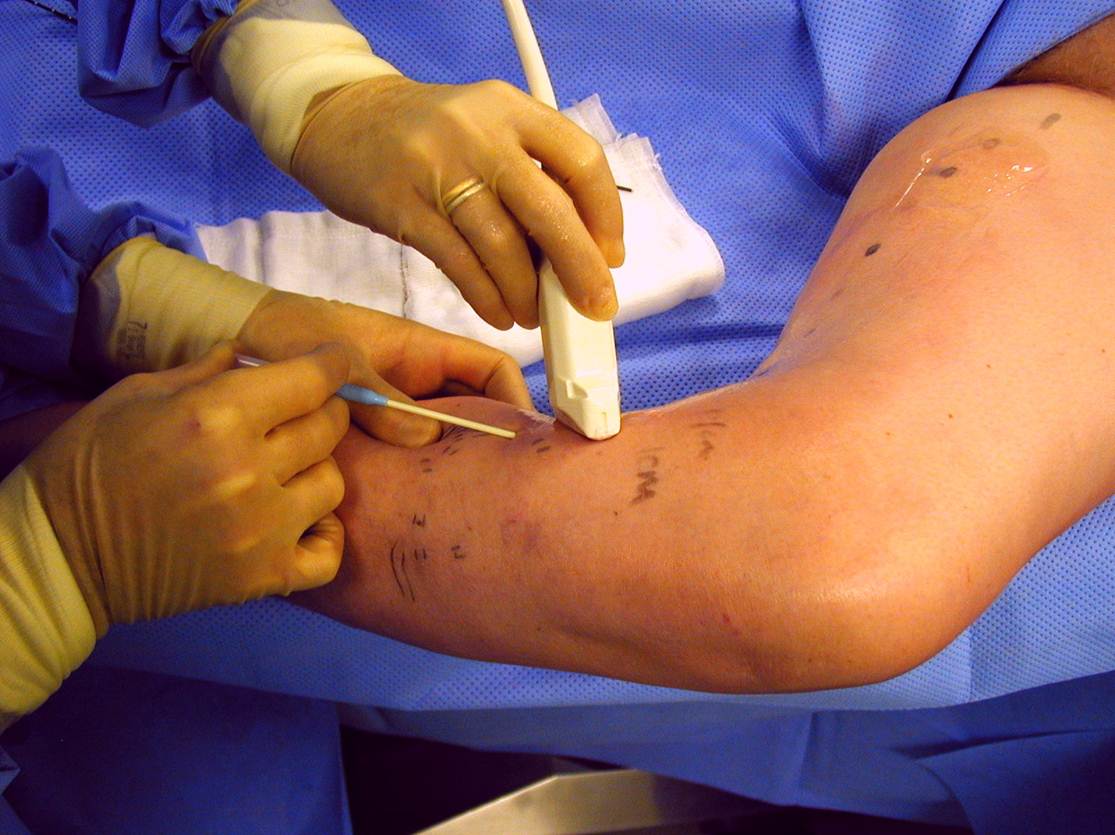
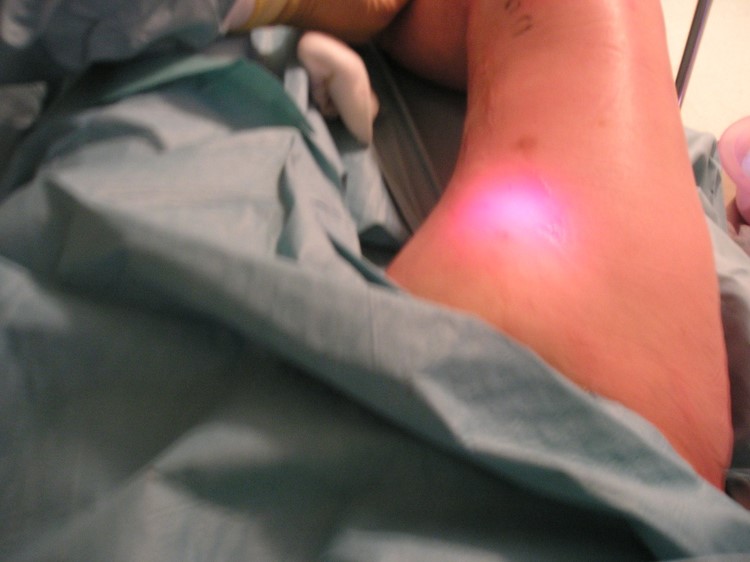 When the catheter is activated in contact with the vein wall either an electrical current or laser energy is passed through the vein wall. This causes the proteins in the vein wall to change shape and contract down. The catheter is slowly pulled back down the vein. This leaves the vein contracted down and no blood flows through it. It is effectively removed from the circulation achieving the same outcome that stripping of the vein does in traditional surgery. Long term follow up has shown that the veins largely remain closed off and rarely open up again.
When the catheter is activated in contact with the vein wall either an electrical current or laser energy is passed through the vein wall. This causes the proteins in the vein wall to change shape and contract down. The catheter is slowly pulled back down the vein. This leaves the vein contracted down and no blood flows through it. It is effectively removed from the circulation achieving the same outcome that stripping of the vein does in traditional surgery. Long term follow up has shown that the veins largely remain closed off and rarely open up again.
Further new ways of occluding the LSV and SSV are being introduced. A form of glue can be used to seal the vein off. This requires no anaesthetic which may be a benefit. The long term durability of this treatment is under evaluation.
Phlebectomy or Avulsion of veins.
The actual lumpy surface varicosities can be removed or "pulled out", by small surgical procedures. This is usually done through a series of small cuts (2-4mm). The terms "avulsions" or “phlebectomy” are used to describe this. The veins are removed in sections (avulsed) through each of the incisions.
After Care
Most procedures are now day case or clinic treatments. Staying overnight is rare. The leg(s) will be firmly bandaged to reduce bruising and help healing. After 1-2 days the bandage may be changed for a stocking which is worn for 5-7 days. For the first few days it may be easier to wear the stocking day and night. After this if the leg is comfortable without it at night, you can use the stocking just during the day. Aim to either rest with the leg elevated moving the ankle, or be up on the move around the house and garden. Avoid standing for any long period of time; avoid crossing your legs. A daily walk of 1-2 miles should be possible.
After the ablation procedures the treated deeper vein may become sore after 3-5 days. This is part of the reaction to the treatment and will settle. Anti-inflammatory pain killers will help with the discomfort for a few days. After phlebectomy the small cuts on the leg will usually be closed with skin glue or tape rather than stitches. Where stitches are used they are usually dissolvable.
Complications
Recovery from RFA or EVLA alone without any phlebectomies can be quite quick in 2-4 days. Phlebectomies in addition will inevitably produce some bruising and soreness. The severity depends on how many veins are removed. Most of the soreness will settle in 3-5 days. Full clearance of the bruising will take longer. Small nerves next to the veins can be disturbed leading to patches of numbness in the lower leg and foot in approximately 10% of patients. This slowly resolves but is occasionally permanent. A thrombosis can occur in the deeper veins of the leg (DVT) but this is not common, affecting less than 1% of patients. Keeping mobile after the procedure and wearing the stocking help reduce the risk of this. Infections in the very small wounds are uncommon.
For more information click HERE
For more detailed information on the evidence for these new procedures see the attached PDF